
Get to know us! Lauren
The latest in our 5 minute chat series is here! We find out what our staff love about the Central Coast and of course, Albany
The team at Albany Dental can treat gum disease, sleep apnea, teeth grinding and more.
Visit our Gosford clinic today to resolve your dental issue!



The latest in our 5 minute chat series is here! We find out what our staff love about the Central Coast and of course, Albany

We’ve all been there: standing in front of the bathroom mirror, toothbrush in hand, pondering the age-old question. Which brushing technique is best? Up and

The latest in our 5 minute chat series is here! We find out what our staff love about the Central Coast and of course, Albany

The latest in our 5 minute chat series is here! We find out what our staff love about the Central Coast and of course, Albany

Toothpaste is a heavily researched and widely produced product that is essential in the effective cleaning of teeth on a daily basis. Since it is

The latest in our 5 minute chat series is here! We find out what our staff love about the Central Coast and of course, Albany

The latest in our 5 minute chat series is here! We find out what our staff love about the Central Coast and of course, Albany
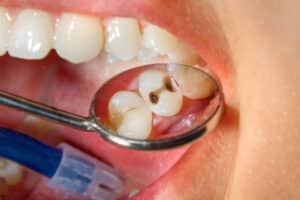
Tooth decay, also known as cavities, is a common dental problem. While the concept seems simple, the progression and treatment options can be intricate. Understanding
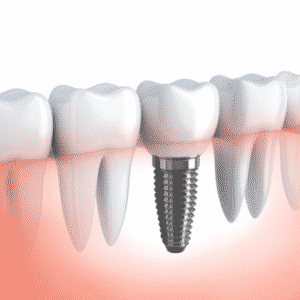
Losing a tooth can be a distressing experience, affecting not just your appearance but also your self-confidence. Dental implants have revolutionised the way we approach
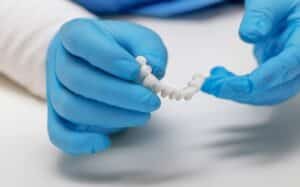
For many of us, a confident smile can truly be the gateway to new opportunities and improved self-esteem. Whether it’s for an important job interview,
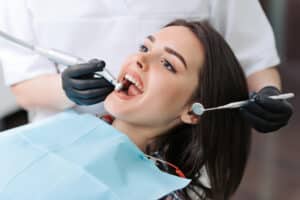
Sometimes life can throw you a curveball in the form of a little dental discomfort. Perhaps you’ve been experiencing some persistent pain at the back

If you’re about to have a tooth extracted for the first time, it’s understandable that you may have some questions. While not everyone wants to
| Monday | 8:30am – 6:30pm |
| Tuesday | 8:30am – 5:30pm |
| Wednesday | 8:30am – 6pm |
| Thursday | 8:30am – 5pm |
| Friday | 8:30am – 3pm |
| Saturday | Closed |
| Sunday | Closed |
Contact Us
